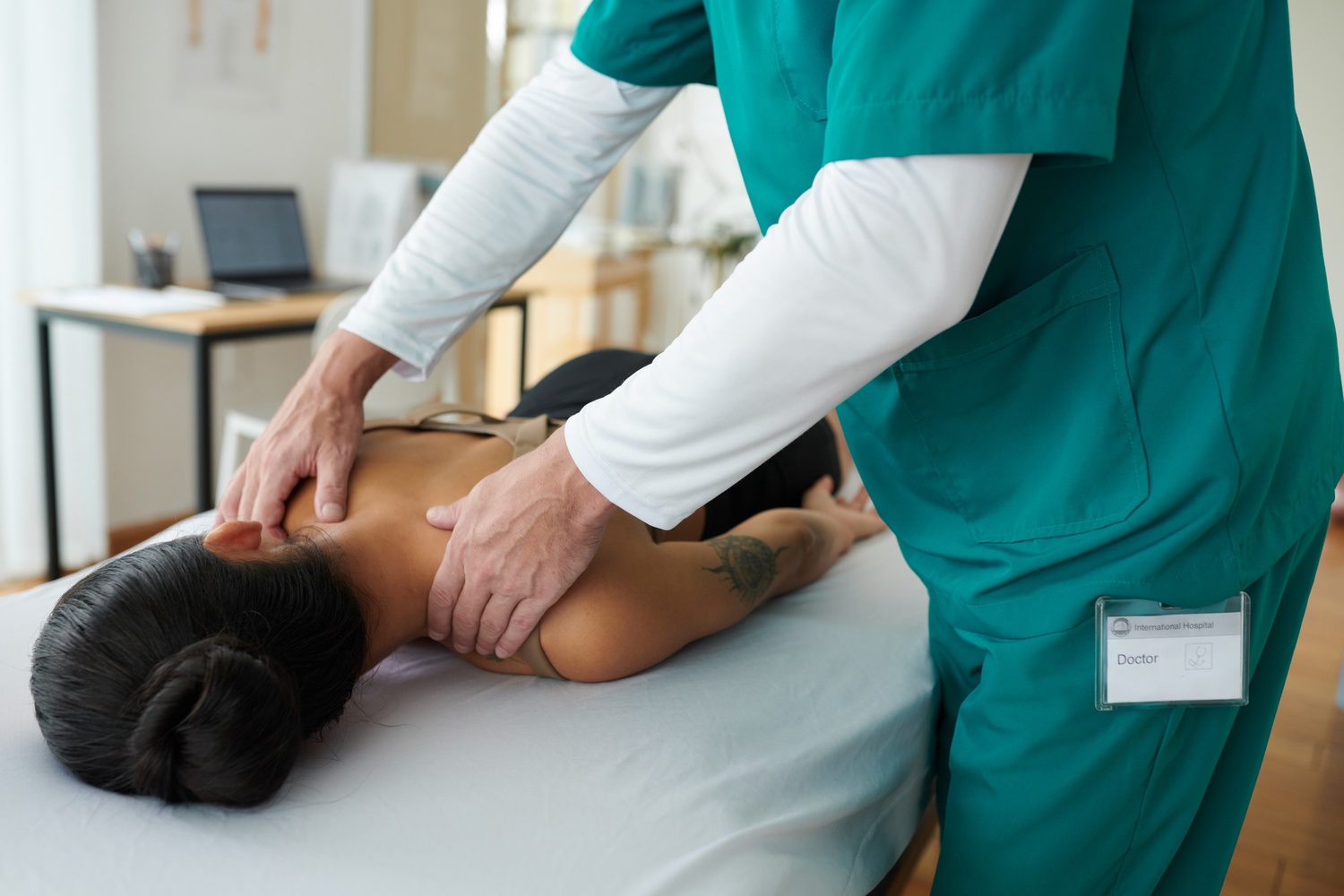
You’ve been told by your GP that you have bursitis in your shoulder, but what exactly is bursitis and what does it mean for you?
Most clients with shoulder bursitis will often present to our clinic with an ultrasound in hand that was ordered by their GP or previous healthcare provider, but often have no idea what it actually is!
Bursa: tiny, fluid filled sac. Itis; inflammation.
Many people with bursitis are often recommended to rest and avoid using their shoulder for 4-6 weeks with the impression that their pain and discomfort will subside. Unfortunately, this rarely happens.
We often tell our clients that bursitis is like an airbag in a car…it doesn’t go off unless something else has happened.
Whether it be tissue damage from a rotator cuff tear, glenohumeral labral damage, loading issues or maybe fascial disturbances elsewhere in the body - there is always a cause that leads to bursitis.
Treat the problem, not the bursitis and more than likely you will see improvement in your symptoms.
What Causes Shoulder Bursitis?
Shoulder bursitis rarely occurs in isolation. In most cases it’s the result of an underlying structural or mechanical problem that creates excessive friction or compression on the bursa. Common causes include:
- Rotator cuff weakness or tears — When the rotator cuff muscles fail to hold the humeral head down during arm elevation, the subacromial space narrows and compresses the bursa.
- Poor shoulder mechanics — Muscle imbalances, tight chest muscles, and rounded posture alter how the shoulder joint moves, increasing impingement of the bursa.
- Repetitive overhead activity — Trades, swimming, tennis, and gym exercises performed with poor technique are common culprits.
- Direct trauma — A fall onto the shoulder or a direct blow can acutely inflame the bursa.
- Age-related changes — Degenerative changes to the rotator cuff tendons reduce the available space in the shoulder, making the bursa more susceptible to compression.
Recognising the Symptoms
The hallmark symptom is a sharp, catching pain when lifting the arm out to the side or above shoulder height — typically between 60 and 120 degrees of elevation, known as the “painful arc.” Other common symptoms include:
- Aching pain at rest, particularly when lying on the affected shoulder at night
- Tenderness on the outside (lateral) aspect of the upper arm
- Pain radiating down the upper arm toward the elbow
- Weakness and reduced range of motion
- Difficulty with everyday tasks: reaching into overhead cupboards, putting on a jacket, or fastening a seatbelt
These symptoms often develop gradually over weeks or months rather than appearing suddenly — which is why many people delay seeking treatment, only to find the problem has worsened.
Why Rest Alone Won’t Fix Shoulder Bursitis
Bursitis is a symptom, not the root cause of your problem. Resting the shoulder may reduce acute pain and inflammation temporarily, but if the underlying mechanical dysfunction causing the bursa to be compressed isn’t corrected, the pain will return — often worse than before.
Anti-inflammatories and cortisone injections can offer short-term relief, but without rehabilitating the structures that caused the problem, patients often find themselves in a revolving door of symptom management rather than genuine recovery. Research consistently shows that exercise rehabilitation targeting the rotator cuff produces better long-term outcomes than passive treatments alone.
How We Treat Shoulder Bursitis at Continuum
Our approach begins with a thorough assessment — not just of the shoulder, but of the entire kinetic chain. We look at shoulder blade control, thoracic spine mobility, rotator cuff strength, and movement patterns to identify the specific mechanical fault driving your symptoms.
Treatment typically involves:
- Manual therapy — Targeted joint mobilisation and soft tissue techniques to restore normal shoulder mechanics and reduce pain
- Exercise rehabilitation — A progressive program to strengthen the rotator cuff and shoulder stabilisers, correcting the muscle imbalances that led to the bursitis
- Load management — Guidance on modifying activities during recovery so you stay active without perpetuating the problem
- Postural correction — Addressing thoracic spine position and scapular control that often contribute to subacromial impingement
Our North Strathfield clinic serves patients from Burwood, Strathfield, Homebush, and across the inner west. If you’ve been told you have shoulder bursitis and haven’t seen improvement with rest, we can help you understand what’s actually driving your pain and build a path to lasting recovery.
Frequently Asked Questions
How long does shoulder bursitis take to heal?
With appropriate treatment addressing the root mechanical cause, most patients see significant improvement within 6–12 weeks. Mild cases resolve faster; cases involving rotator cuff pathology or significant degenerative changes may take longer. Without treatment, bursitis often becomes chronic and progressively more limiting.
Should I get a cortisone injection for shoulder bursitis?
Cortisone injections can be appropriate for managing severe pain in the short term, but they don’t address the mechanical cause of the bursitis. Research suggests cortisone provides better short-term pain relief but no better long-term outcomes than manual therapy and exercise rehabilitation. We typically recommend conservative management first, with cortisone reserved for cases where pain is preventing participation in rehab.
Can shoulder bursitis come back after it heals?
Yes — and it commonly does, particularly if the underlying cause wasn’t fully addressed. This is why rehabilitation targeting strength, movement patterns, and posture is essential, not just pain relief. Patients who complete a full rehabilitation program have much lower rates of recurrence than those who stop treatment once pain settles.
Is shoulder bursitis the same as a rotator cuff tear?
No — they are different conditions, though they frequently co-exist. Bursitis is inflammation of the bursa sac; a rotator cuff tear is a structural injury to one of the four rotator cuff tendons. Rotator cuff pathology is one of the most common causes of bursitis, which is why a thorough assessment is essential to understand exactly what’s driving your symptoms.
If you’ve been diagnosed with shoulder bursitis, don’t wait for it to resolve on its own. Learn more about subacromial impingement syndrome — the condition most closely linked to shoulder bursitis — or book an appointment with our team to get a clear, honest picture of what’s causing your pain and how to fix it.
You may also be interested in
Sports & Recreational Activities Injuries Statistics Australia
Staying active is part of the Aussie lifestyle, yet these activities bring…
How Much Does Chiropractic Treatment Cost in Sydney?
Chiropractic care is very popular in Australia. In fact, it is regarded as a…
Dry Needling Statistics Australia: Facts & Insights
Dry needling has gained traction recently, yet it is nearly identical to…